Researchers at UC Davis Health have uncovered a consistent brain chemistry marker in people with anxiety disorders: significantly lower levels of choline, an essential nutrient tied to memory, mood, and nerve function.
The discovery emerged from a meta-analysis of 25 prior studies examining brain chemistry in 370 people with anxiety disorders and 342 without. The analysis found that anxious individuals had roughly 8% lower choline concentrations in their brains, with the pattern most pronounced in the prefrontal cortex, the region responsible for emotional regulation and decision making.
"This is the first meta-analysis to show a chemical pattern in the brain in anxiety disorders," said Jason Smucny, co-author and assistant professor in UC Davis's Department of Psychiatry and Behavioral Sciences. "It suggests nutritional approaches, like appropriate choline supplementation, may help restore brain chemistry and improve outcomes for patients."
Choline plays critical roles throughout the body. It helps construct cell membranes and supports brain functions central to memory, mood regulation, and muscle control. While the body produces small amounts on its own, the vast majority must come from dietary sources.
Anxiety disorders represent the most common mental illness in the United States, affecting roughly 30% of adults, according to the study's senior author Richard Maddock, a psychiatrist and research professor at UC Davis. The conditions, which include generalized anxiety disorder, panic disorder, and various phobias, often leave people struggling with excessive worry and difficulty controlling fear responses.
The brain's anxiety response hinges on two key regions working in tandem. The amygdala shapes the sense of threat or safety, while the prefrontal cortex manages planning and emotional control. In anxiety disorders, this balance shifts dangerously. Ordinary concerns feel overwhelming, and the body's stress response becomes hard to deactivate.
Neurotransmitters play a crucial role in this imbalance. Norepinephrine, which drives the body's fight-or-flight response, typically runs elevated in anxiety disorders. The UC Davis researchers theorize that this heightened arousal increases the brain's demand for choline. If the brain cannot obtain enough to meet that surge in demand, choline levels may plummet.
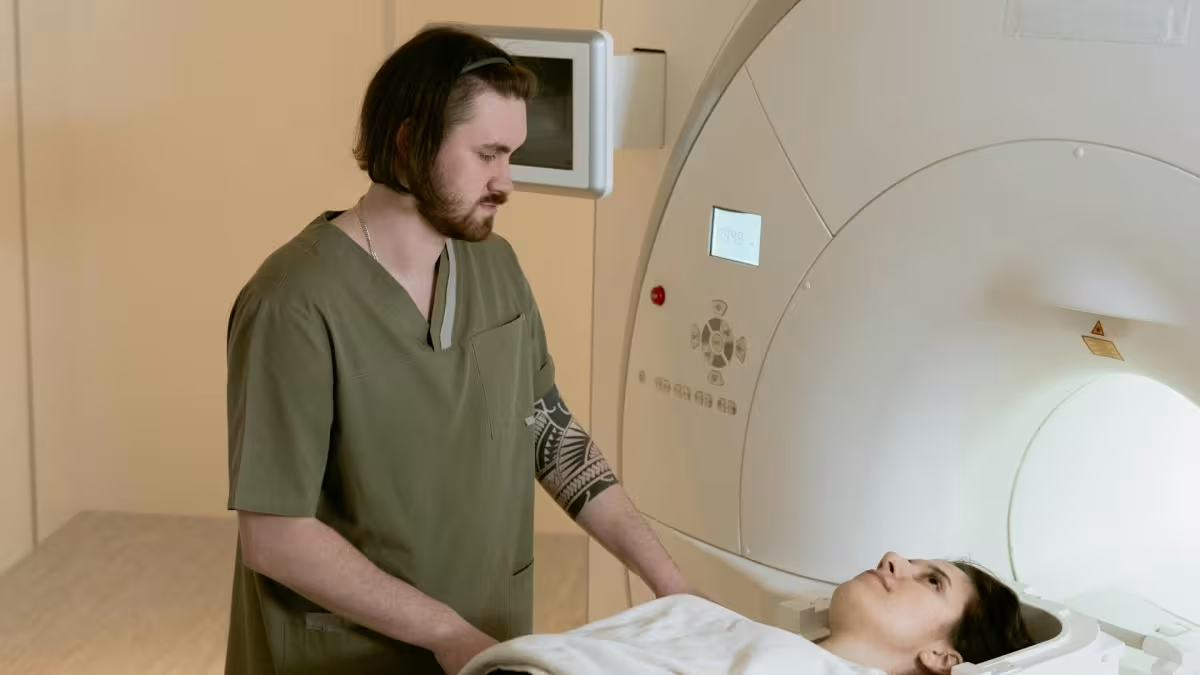
Maddock and Smucny measured brain chemistry using proton magnetic resonance spectroscopy, a noninvasive technique performed within an MRI machine. Rather than producing standard images of brain structure, this method uses magnetic fields and radio waves to quantify chemical levels in tissue. Maddock had previously observed low choline in people with panic disorder, prompting the larger meta-analysis. The consistency of the 8% reduction across different anxiety diagnoses caught the researchers' attention.
"An 8% lower amount doesn't sound like that much, but in the brain it's significant," Maddock said.
The analysis also detected reduced levels of NAA, a marker generally considered indicative of neuronal health, across brain regions. However, the choline reduction emerged as the clearest and most uniform signal across all anxiety disorders studied.
The findings do not yet prove that low dietary choline causes anxiety or that supplementation will relieve symptoms. Maddock stressed the need for caution. "We don't know yet if increasing choline in the diet will help reduce anxiety. More research will be needed," he said. He warned against self-medication with excessive choline supplements.
Still, the discovery aligns with growing research interest in nutrition's role in mental health. Many Americans, including children, fail to consume the recommended daily amount of choline. Maddock suggested that people with anxiety might examine their diets to ensure adequate choline intake. Omega-3 fatty acids found in salmon may prove especially beneficial for delivering choline to the brain.
Foods rich in choline include beef liver, eggs (particularly the yolk), beef, chicken, fish, soybeans, and milk.
Related research has produced mixed results. One dietary study found that higher choline intake correlated with lower depression odds in adults but showed no significant link to anxiety or psychological distress when adjusted for other factors. That makes the UC Davis brain imaging finding particularly striking: it points to a measurable chemical difference inside the brain without yet proving causation or treatment efficacy.
Controlled clinical trials would be required to test whether altering choline intake can change brain chemistry or improve anxiety symptoms. For now, researchers suggest that nutrition likely represents one piece of a complex puzzle, but not a substitute for professional mental health treatment.
Author Jessica Williams: "The choline finding is intriguing, but let's not mistake a chemical marker for a cure, especially when researchers themselves are being careful not to oversell the implications."
Comments